Understand Success Rates and Help Keep Your Surrogacy Journey On Track
This article originally appeared in Fertility Road magazine and online at FertilityRoad.com.
Craig Reisser, a parent via egg donation and surrogacy in the USA, shares some advice for intended parents on how to use success rates when planning your surrogacy journey.
When it comes to choosing an IVF clinic a discussion of success rates is sure to be one of the key considerations.
Success rates can be a notoriously complicated area for intended parents, not only because there can be so many factors that play a part in them, but also because clinics may report them in any number of ways. I certainly found this to be true when I was undertaking my own journey.
Because your IVF clinic will play a pivotal role in shaping your journey, understanding how to make sure you are focussing on the right success rates for the specific IVF procedure you are planning, as well as how to apply them in a practical manner to your decision making is essential.
In my view, your ideal goal with IVF should be to have the best chance of success and a healthy baby on your first attempt. Or in other words, minimizing the risk that you will have to repeat any aspect of the IVF process. This is the best way to keep your budget and timetable under control and your stress levels to a minimum.
While my focus here is on IVF for a surrogacy journey, as this was my own personal experience, this same objective can apply equally to anyone undergoing IVF – whether using her own eggs or donor eggs, working with a surrogate or planning to carry the pregnancy herself.
In an ideal world, first-time success would mean two things. Firstly, only needing one egg retrieval and embryology cycle (including embryo testing if applicable) to obtain all the viable embryos that you will need to build your family. Secondly only needing a single embryo transfer for the live birth of a healthy baby.
For many intended parents, their actual IVF experience does not reflect this ideal and they may require more than one egg retrieval and embryology cycle and/or more than one embryo transfer to achieve their dream of a healthy baby.
Each time that you need to repeat either of these steps in the IVF process there are real implications for you in terms of higher costs, a longer timetable, and added emotional stress.
The real “value of success” is therefore that higher success rates can help you avoid costs, keep your timeline to a minimum, and your stress levels in check.
Intended parents, therefore, need to know which success rates to focus on, how to apply them to make practical choices, and what they mean in terms of the likely number of times they will have to undergo each step of the IVF process to reach their goal.
With this in mind, I focus on two key elements of the IVF process where achieving first-time success can make a real difference in your journey: the egg retrieval and embryology cycle and the embryo transfer. These steps are distinct but intimately connected.
My focus on these two aspects is not meant to diminish the importance of other elements of the IVF process that can play a part in having a healthy baby, such as genetic screening and the choice regarding the number of embryos to transfer, and which intended parents should also consider.
Egg Retrieval and Embryology Cycle
 In my view, the real measure of success for an egg retrieval and embryology cycle is the number of viable embryos obtained, and whether this meets or exceeds the number that you can expect you may need.
In my view, the real measure of success for an egg retrieval and embryology cycle is the number of viable embryos obtained, and whether this meets or exceeds the number that you can expect you may need.
The number of viable embryos that you may need depends on how many children, over time, you hope to have multiplied by the number of transfers you can expect will be required to achieve a live birth. If you plan to transfer more than one embryo at a time, then this needs to be factored in as well.
It’s certainly true that you only need one viable embryo to have a child and success on the first embryo transfer can absolutely happen. However, the reality is that that embryo transfer success rates are not 100%. Therefore there is a potential risk that you may need to repeat the egg retrieval and embryology cycle if you only have a single embryo at the end of this step in the IVF process.
For example, if you hope for one child and can expect that you may need to undergo two transfers to achieve a live birth, then you will hope to have at least two viable embryos. If say, however, you hope to also have a sibling in the future for your first child (and can expect that again you may need to undergo two transfers to achieve a live birth) then you will hope to have obtained at least four viable embryos from your egg retrieval and embryology cycle in order to minimise the risk of needing to repeat this step to create more embryos.
The egg retrieval and embryology cycle is the most expensive part of the IVF process to have to repeat. It may represent some 75-80% percent of the IVF costs of a single successful journey. In addition to the medical costs, you may incur for a repeat cycle, if you are using an egg donor there will also be donor compensation and potentially travel reimbursement, as well as possibly egg donor agency fees and screening costs that may need to be paid again.
Depending on when this step would need to be repeated, and possible scheduling considerations, (e.g. egg donor availability) it could lengthen your timeline from a few to several months.
Unfortunately, for intended parents, the public databases for clinic success rates (such as SART and the CDC in the USA) do not report the statistics, namely the average number of viable embryos that each cycle type has achieved at a clinic, which could help inform intended parents’ decisions.
Though each cycle is unique and some factors cannot be controlled, IVF clinics should have this type of success data, particularly in the case of egg donor cycles. You should be sure to ask about this, as well as the factors that contribute to successful egg retrieval and embryology cycles, including stimulation and egg retrieval medical protocols, the quality of the embryology laboratory, and the role of ovarian reserve. This will help you in making decisions that may help you increase the chance of first-time success.
Embryo Transfer
Beneficially for intended parents, the public databases for clinic success rates generally focus on the statistics that help them understand the chance of success with an individual embryo transfer.
Live Birth Rate Per Transfer, is the relevant success rate to focus on as it represents your ultimate goal. Where more than one embryo has been transferred, a Live Birth Rate Per Transfer will refer to the birth of at least one child.
Sometimes, clinics may instead quote Pregnancy Rate Per Transfer. This represents the percentage of embryo transfers that had an ongoing pregnancy when the rate was calculated. This is not the same as the Live Birth Rate Per Transfer as some pregnancies that were ongoing when the success rate was calculated will not progress. As a result, this measure will be a few to several points higher than the one that matters most for you.
Occasionally some clinics may report their success rates on a cumulative rather than a per transfer basis. Cumulative success rates calculated over multiple embryo transfers will be higher in comparison to per transfer success rates.
Cumulative rates can be helpful if understood correctly, but intended parents may be confused in thinking that a Live Birth Rate presented on a cumulative basis is comparable to one presented on a per transfer basis. For example, a 67% Live Birth Rate Per Transfer will represent a much greater chance of success on the first transfer attempt (and therefore a lower cost and shorter timeframe) than a 67% Cumulative Live Birth Rate calculated over say three transfers.
Generally speaking, it takes more than one embryo transfer to achieve a live birth. So from a practical point of view, you may want to translate the Live Birth Rate Per Transfer into an estimation of the number of embryo transfer attempts you may actually need in order to achieve a live birth. It is this number of expected embryo transfer attempts that will influence the number of viable embryos you should hope to obtain from your egg retrieval and embryology cycle. It will also impact how you plan your budget and timetable.
If an embryo transfer needs to be repeated then this will add to your timeline and costs. Extra costs may include the transfer procedure itself and related medications, pre and post-transfer monitoring, as well as other costs such as travel.
You can estimate the potential number of embryo transfers you may need to achieve a live birth. Using the Live Birth Rate Per Transfer, you can calculate the cumulative probability that you will have a live birth within a certain number of transfers.
In the example below, using a Live Birth Rate Per Transfer of 50%, intended parents would have an 88% chance of having a live birth within 3 transfers. They may get lucky and have a live birth on the first or second transfer, and there still remains a small chance that they will not have been successful by the third transfer. This type of calculation can help intended parents plan for the possible implications to their budget and timeline of their IVF clinic’s success rate.
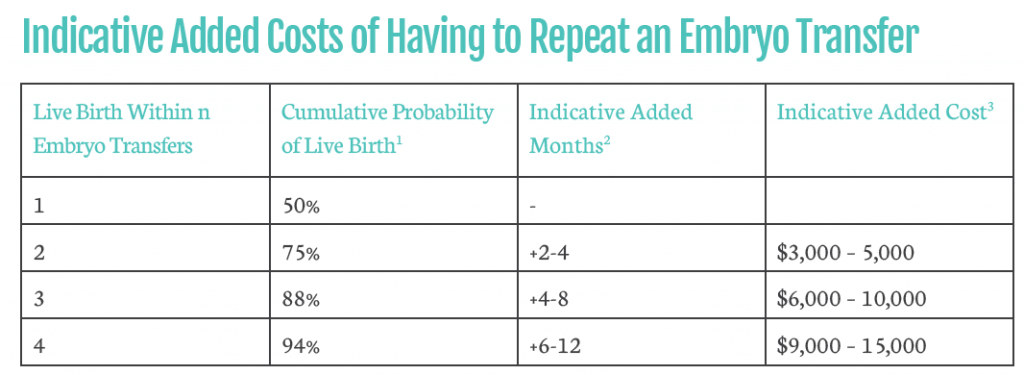
- Based on the SART-reported US National Live Birth Rate Per Transfer in 2016 for all donor egg + surrogacy frozen embryo transfers.
- 2-4 months in an indicative period of time to prepare for and undergo a repeat embryo transfer.
- $3,000 – 5,000 is an indicative additional cost of elements associated with a repeat embryo transfer. If an additional egg retrieval and embryology cycle were needed these costs would be extra.
 Success the First Time
Success the First Time
In my family’s own journey we found that this type of understating of success rates helpful. It focussed us on the factors that would help keep our journey on track, namely obtaining the highest number of viable embryos and minimizing the number of required transfers. It also allowed us to plan our budget and timeline, accounting for the probability that we might have to repeat either step in the IVF process. Thankfully, we had the first time success that we were hoping for and I believe that the decisions we made, armed with this understanding, played a big part in this.
US IVF Success Rate Resources
For those intended parents looking at IVF treatment in the USA, there are two online, public databases that contain national and individual US IVF clinic success rates – The US Society for Assisted Reproductive Technology (SART) at www.SART.org and the US Centers for Disease Control (CDC) at www.cdc.gov/art.
SART has been recording US IVF clinic success rates since 1988. Additionally, since 1992 all US IVF clinics have been mandated by the US government to report their success rate data to the CDC. SART membership is voluntary for US IVF clinics. About 80% of US IVF clinics are SART members and about 95% of US IVF cycles are captured in the SART success rate database.
 Both SART and the CDC have now released the 2016 live birth success rates for US IVF procedures and this represents the most current US live birth success rates. The 2016 data is available alongside the 2015 data for year-on-year comparisons. The 2017 live birth rate data will be known and reported in the Spring of 2019.
Both SART and the CDC have now released the 2016 live birth success rates for US IVF procedures and this represents the most current US live birth success rates. The 2016 data is available alongside the 2015 data for year-on-year comparisons. The 2017 live birth rate data will be known and reported in the Spring of 2019.
The SART database allows for easy filtering by clinic for specific procedure types – surrogacy, egg donation, PGS/PGD testing, and more – as well as for the specific number of embryos transferred.
This functionality is a real benefit for intended parents considering US IVF clinics as they can now search for live birth success rates for the exact procedure they are seeking to undergo by clinic, as well as US national averages for comparison. It also allows them to view consistently prepared and presented data and live birth success rates for every clinic they may be considering. It allows them to reference a clinic’s 2016 data to its 2015 results as well to national statistics for both periods.
Craig is a regular contributor to Fertility Road on third-party reproduction. Look for his upcoming articles on egg donation and surrogacy in future issues of Fertility Road or contact him at oregonreproductivemedicine.com.



